
On behalf of our entire Key Ministry team, I’m delighted to announce that Inclusion Fusion Live, the disability ministry conference we’ve hosted annually is currently scheduled to take place as a live and “in person” event on Saturday, April 17th, originating from Bay Presbyterian Church in suburban Cleveland. The theme of this year’s conference is doing ministry together after the pandemic.
Over the past year, some of our friends and colleagues in ministry put forth heroic efforts in producing very comprehensive online conferences with some of the best teaching on disability ministry we’ve seen anywhere. We were honored as a team to have participated in the Wonderfully Made and All Access conferences, as well as an Online Pastors Retreat loaded with mental health ministry resources. We don’t need to replicate their efforts – churches and ministry leaders interested in that training can readily access it by reaching out to the organizers of those events. Our team senses that the moment calls for something different.
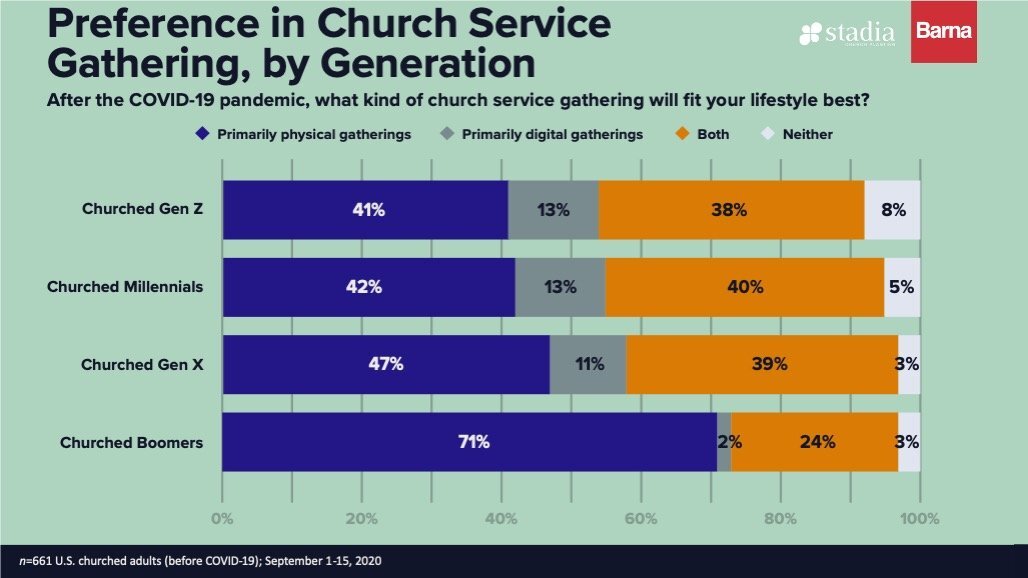
Our understanding and experience of “church” has been shaken to an extent unlike any of us have experienced in our lifetimes. Months after most churches reopened for in-person worship, attendance at two-thirds of churches in the U.S. is down at least 30%, at least 50% in three churches out of ten and over 70% in one church in ten. Individuals and families served by our ministries have been among those most impacted by social isolation and their medical vulnerabilities will cause them to be among the last to return to church.
We think it’s important at this moment for as many of us as possible to gather together in the physical presence of others (with appropriate health and safety precautions and social distancing) who share our love for Jesus and passion for including families impacted by disability in the church. We need to be with one another! It’s only through tapping the collective gifts we’ve received through the Spirit that we’ll be effective in our calling and help lead the larger church as it seeks to recapture the people and cultural influence lost in recent years – losses greatly accelerated by the pandemic.
Some things about #IFL2021 will be as they have in the past – we’re gathering in Cleveland during spring to share ideas, hang out with one another and prepare for a new season of ministry. As with so many things in life this past year, much will be different.
In order to minimize risks associated with travel and promote a sense of connection and community between disability ministry leaders within cities and regions, #IFL2021 will be a live, multisite event. We’re expecting between 10-25 attendees at each site, possibly more at sites with the ability to host larger numbers safely.
This year’s conference will be one day as opposed to two to minimize the COVID – related burdens on our host sites.
Unlike past conferences that sought to provide education and resources on a broad variety of ministry topics, #IFL2021 will be organized around ONE theme. Disability ministry in the aftermath of the pandemic.
Because we’re seeking to tap into collective wisdom, there are no individual talks or presentations this year. #IFL2021 will be organized around seven conversations. Everyone attending in person will participate actively in these conversations. We’ll have familiar faces on our stage in Cleveland kicking off each conversation, which will be shared via webcast to each host site. Host sites will have one or more facilitators who will continue the conversations with attendees at their sites, emphasizing idea-sharing and development of local collaborations and solutions. We’ll have a livestreaming option for participants unable to attend an in-person event at this time. They will be placed in video discussion groups organized by region.
Out of the seven conversations, one – our “featured conversation” will be prerecorded. We wanted our friend and colleague Lamar Hardwick to facilitate the conversation sparked by his new book on the central role disability – and ministry leaders with disabilities should play in the dialogue around diversity in the church but thought it unwise to ask him to travel while he’s undergoing treatment for colon cancer. The disability and diversity conversation will kick off the conference in the Eastern and Central time zones and conclude the day in the Mountain and Western time zones.
Other topics of conversation we’ll likely address include…
How might our churches best address the need for Christian community among families impacted by disability already marginalized before the pandemic?
How might innovative practices resulting from COVID shape disability ministry going forward?
How can we preserve and support ministries struggling from a lack of funding or volunteers?
How might we promote collaboration within regions between churches and organizations engaged in disability ministry?
How might we best address the training needs of church staff, disability ministry leaders and volunteers going forward?
How can we help the church minister with the rapidly growing population impacted by mental health issues?
To make #IFL2021 a reality, we’re going to need help from lots of friends. Would your church consider serving as a host site for the conference? Click here if you’re interested in learning more about hosting. After you provide us with some basic information, a member of our team will be in touch shortly to discuss hosting requirements and the services and supports we provide. We’re hoping to open individual registration for #IFL2021 by March 21st. We understand the timeline is tight, but we quickly learned while refunding registrations for last year’s conference that advance planning during COVID is often futile.
We miss our friends and colleagues. We’re looking forward to seeing members of our “tribe” and affording friends here in Cleveland and around the country with opportunities to reconnect for the purpose of identifying collective solutions to the ministry challenges we’re facing in the months and years to come.
We encourage everyone to follow Key Ministry’s Facebook page, our family support page or contact us to receive updates on #IFL2021 and other ministry programming and activities.


























 Heather Sells (CBN News) will interview prominent pastors and ministry leaders who discuss their personal experiences with mental health and share their observations about the best ways to minister to those navigating mental and emotional health issues. Guests include Dr. Jack Graham (Prestonwood Baptist Church), Amy Simpson (Author of Troubled Minds), Joe Padilla, (Mental Health Grace Alliance), Brad Hoefs, Founder of Fresh Hope for Mental Health and Dylan Dodson, (New City Church, Raleigh, NC). In a separate presentation, Pastor Dodson discusses practical strategies for walking through tragedies with people in your church.
Heather Sells (CBN News) will interview prominent pastors and ministry leaders who discuss their personal experiences with mental health and share their observations about the best ways to minister to those navigating mental and emotional health issues. Guests include Dr. Jack Graham (Prestonwood Baptist Church), Amy Simpson (Author of Troubled Minds), Joe Padilla, (Mental Health Grace Alliance), Brad Hoefs, Founder of Fresh Hope for Mental Health and Dylan Dodson, (New City Church, Raleigh, NC). In a separate presentation, Pastor Dodson discusses practical strategies for walking through tragedies with people in your church. Brad Hambrick (Pastor of Counseling at The Summit Church in Durham, NC) will be discussing how to use the Bible effectively with someone who has experienced trauma. His presentation has been designed for anyone who provides pastoral care with victims of abuse, first responders (police officers, medical professionals, etc.), persons serving in the military or couples who have lost a child.
Brad Hambrick (Pastor of Counseling at The Summit Church in Durham, NC) will be discussing how to use the Bible effectively with someone who has experienced trauma. His presentation has been designed for anyone who provides pastoral care with victims of abuse, first responders (police officers, medical professionals, etc.), persons serving in the military or couples who have lost a child. Ben O’Dell (Mental Health Liaison for the HHS Center for Faith and Opportunity Initiatives) will introduce the Partnership Center’s Compassion in Action Guide – a compendium of resources, “best practices,” and innovative services to help pastors and other church staff to address mental illness in their churches and communities. The guide presents seven key principles to implementation of mental health support.
Ben O’Dell (Mental Health Liaison for the HHS Center for Faith and Opportunity Initiatives) will introduce the Partnership Center’s Compassion in Action Guide – a compendium of resources, “best practices,” and innovative services to help pastors and other church staff to address mental illness in their churches and communities. The guide presents seven key principles to implementation of mental health support. Evan Owens (Reboot Recovery) will be sharing a presentation for pastors and church leaders designed to help those who minister with first responders and their loved ones assist them in healing from the moral and spiritual wounds associated with service-related trauma during a time in which COVID-19, civil unrest and a barrage of economic challenges have pushed many heroes to the brink
Evan Owens (Reboot Recovery) will be sharing a presentation for pastors and church leaders designed to help those who minister with first responders and their loved ones assist them in healing from the moral and spiritual wounds associated with service-related trauma during a time in which COVID-19, civil unrest and a barrage of economic challenges have pushed many heroes to the brink Dr. Matthew Stanford (Hope and Healing Institute, Houston TX) will be providing an overview of their Gateway to Hope (GTH) training – an interactive, evidence-based, mental health awareness training and education program offered online free of charge to interested churches. GTH training equips pastors, ministry staff, and volunteers to identify mental health problems early, refer distressed individuals to professional care, offer evidence-based psychoeducational services on site, and provide a therapeutic community to support recovery. He will discuss how churches might use the training to enhance their ability to minister to those living with serious mental illness and their families.
Dr. Matthew Stanford (Hope and Healing Institute, Houston TX) will be providing an overview of their Gateway to Hope (GTH) training – an interactive, evidence-based, mental health awareness training and education program offered online free of charge to interested churches. GTH training equips pastors, ministry staff, and volunteers to identify mental health problems early, refer distressed individuals to professional care, offer evidence-based psychoeducational services on site, and provide a therapeutic community to support recovery. He will discuss how churches might use the training to enhance their ability to minister to those living with serious mental illness and their families.
 In
In 









